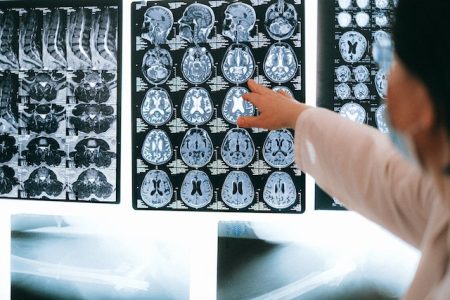
Interpreting results:
Have you ever been sent for a scan and been shocked by the long report that comes with it? The increasing use of Magnetic Resonance Imaging (MRI) means we can get a better picture of our bodies and see in greater detail than ever before.
A Radiographer’s report of your scan will detail every deviation from “normal” but in truth, most of the time, the deviations are part of normal age related changes! Just like our faces do not look the same at 20 as they do at 50; the inside of our bodies will change too.
A lot of what is reported may have been present long before your injury and not contributing to your pain in any way. A number of studies dedicated to investigating this have shown surprising results.
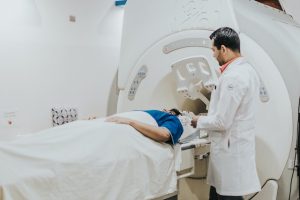
Findings do not always = symptoms:
In a study looking at the knees of 44 people, average age 41 years, with no knee pain, 43 of those people showed at least one meniscal abnormality and 27 people had abnormalities in at least three of the four regions of the knee. 12 people had osteophytes and 5 people had cartilage lesions, 15 people had grade 1 or 2 osteoarthritis. None of them had pain! (Beattie et al 2005).
Another study looking at the knees of 230 asymptomatic people found 97% had abnormalities on MRI. 30% had meniscus tears, 57% had patellofemoral cartilage abnormalities, 48% had patellofemoral bone marrow abnormalities, 50% had moderate to severe cartilage lesions, 50% had moderate to severe bone marrow oedema. Again, none of them had pain. (Horga et al. 2020).
There can be a lot of fear in hearing the term “disc bulge” but a study of over one thousand people aged from 20 to 70 years old, with no neck pain, found that 87.6% had disc bulges in their cervical spine (neck). There was a trend for the disc bulges to increase in severity and number of levels of the spine with increasing age (Nakashima et al., 2015).
How do we know if a finding holds any clinical significance?
From these studies we can see that not every abnormality in our body can cause pain and many “abnormalities” may be better viewed as normal age related changes or variations of the individual. So how do we tell the difference between something on a scan that is contributing to your pain, i.e. something that is clinically significant and something that is not?
Health professionals, including Physiotherapists, use their knowledge of anatomy, pathology and biomechanics to help decipher your pain by asking lots of questions, performing tests and looking at your movement and pain response. They can help work out what is clinically significant and contributes to your pain and what is not clinically significant in your scans.
References:
- Beattie KA, Boulos P, Pui M, O’Neill J, Inglis D, Webber CE, Adachi JD Abnormalities identified in the knees of asymptomatic volunteers using peripheral magnetic resonance imaging Osteoarthritis and Cartilage 2005: 3: 181-186
- Culvenor AG, Ferraz Pazzinatto M, Heerey JJ Infographic. When is abnormal normal? Reframing MRI abnormalities as a normal part of ageing British Journal of Sports Medicine 2021;55:761-762.
- Horga LM, Hirschman AC, Henckel J, Fotiadou A, Di Laura A, Torlasco C, D’Silva A, Sharma S, Moon JC, Hart AJ. Prevalence of abnormal findings in 230 knees of asymptomatic adults using 3.0 T MRI. Skeletal Radiology. 2020; 49(7): 1099–1107
- Nakashima H, MD, Yukawa Y, Suda K, Yamagata M, Ueta T, Kato F. Abnormal Findings on Magnetic Resonance Images of the Cervical Spines in 1211 Asymptomatic Subjects Spine, 2015; 40 (6): 392 – 398
~ Sarah Jarvie
Physiotherapist
You may also find these PMPP blogs interesting:
- https://portmelbournephysio.com.au/does-exercise-reduce-pain/#:~:text=Exercise%20creates%20hormonal%20and%20chemical,endorphins%20and%20serotonin%20following%20exercise.
- https://portmelbournephysio.com.au/the-mri-experience/
- https://portmelbournephysio.com.au/lowbackpain/
- https://portmelbournephysio.com.au/lower-back-radiculopathy/